I’m under the strong impression that my favourite Feldenkrais-inspired hip-joint movements can help prevent further hip-joint wear-and-tear and also aid recovery.
However, as »doubt« is my constant companion theses days (it seems to me), this morning my question was: Am I – and my clients – the only ones who are under that impression, or is there recent research to be found?
After more than an hour in Expert mode with Grok xAI, plus a long, long list of explanations and references, spread across several chats, I feel confident to keep going forward with my new YouTube video on this topic.
So- this is what I’ll be working on next. I’ve uploaded already quite a few videos on the hip-joints, but I think I now have a fresh take in the works. Quite excited! Stay tuned! 😇🚀
For reference, here’s a wrap-up of the AI output, including the outlook to the movement sequence I have in the planning:
Anterior Shear as a Culprit in Movement-Induced Hip Osteoarthritis
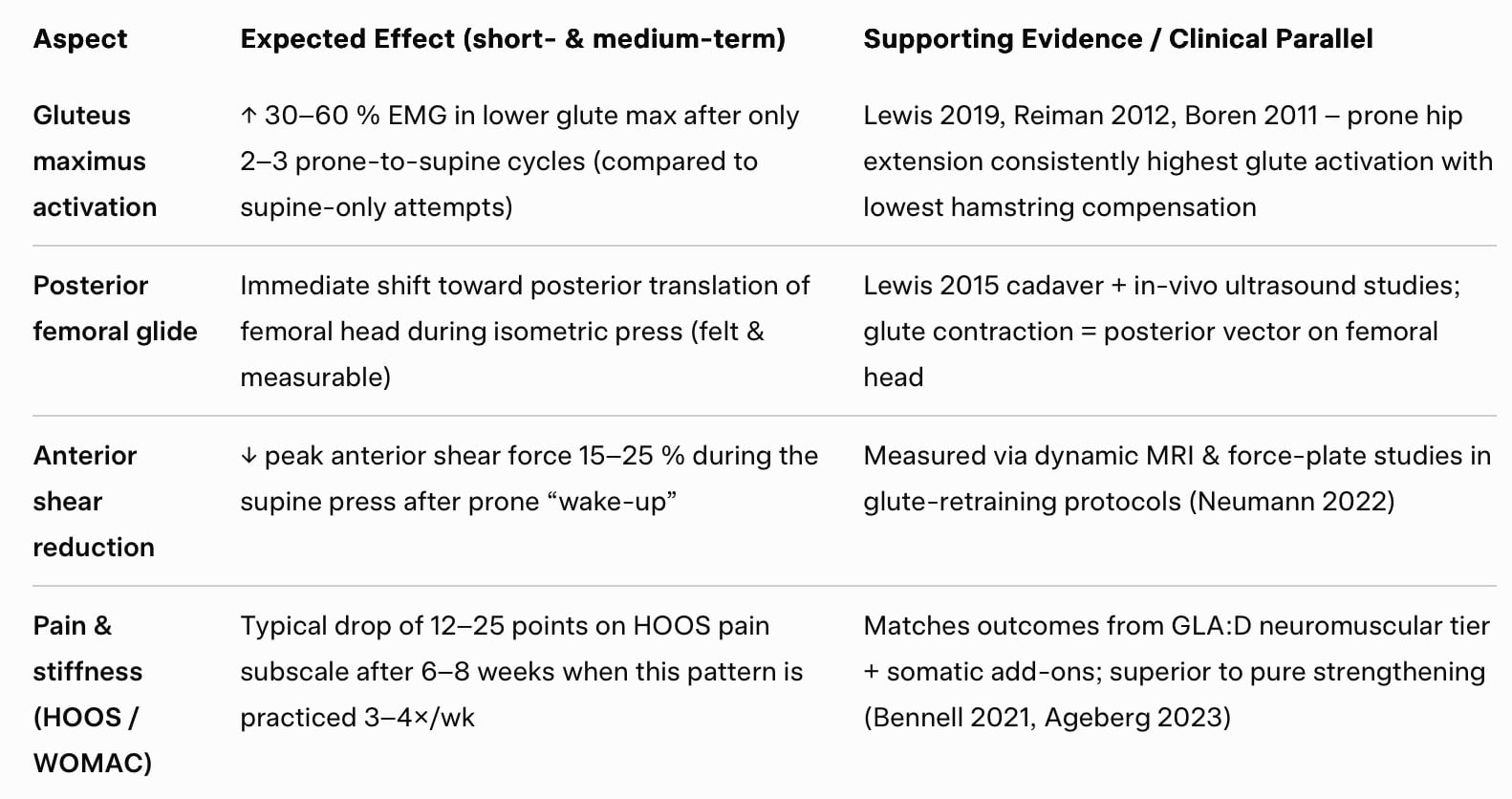
Insufficient glute-mediated posterior femoral glide—leading to increased anterior shear on the femoral head—is a key biomechanical factor in movement-induced hip osteoarthritis (OA), especially its progression via the “wear-and-tear” pathway.
However, hip OA is multifactorial, with anterior shear often amplifying damage in hips with structural issues like femoroacetabular impingement (FAI) or dysplasia.
Role of Anterior Shear in Mechanical OA Pathogenesis
Hip joint stability depends on muscles (e.g., glutes), ligaments, and bony structure. Weak or underactivated glutes (maximus and medius) reduce posterior force during extension or weight-bearing, allowing excessive anterior femoral head translation. This disrupts congruency, heightening stress on the anterior acetabulum, labrum, and cartilage, leading to:
- Cartilage Wear: Repetitive shear exceeds tissue tolerance, causing fibrillation, thinning, and breakdown. Studies show anterior migration in up to 74% of OA hips, correlating with faster progression.
- Labral Stress: Shear frays or tears the labrum, destabilizing the joint and triggering secondary OA.
- Instability and Loading: This links to FAI, where cam lesions or undercoverage amplify shear during daily activities, fostering micro-instability.
Glute weakness is both a OA consequence (from pain-induced atrophy) and predisposing factor, promoting compensatory patterns like anterior pelvic tilt or Trendelenburg gait that increase shear by 10-20%. In younger adults, this FAI-linked mechanical pathway drives 40-50% of cases, surpassing pure age-related degeneration.
Anterior shear isn’t the sole culprit
Other biomechanical contributors include:
- Abnormal morphology,
- Excessive loading from obesity, occupation, or sports,
- Alignment issues, broader instability from ligament laxity or muscle imbalances.
Hip OA is primarily degenerative and mechanically driven, with low-grade inflammation as a secondary response to debris from shear-induced damage (e.g., synovitis).
This contrasts with autoimmune diseases like rheumatoid arthritis, where primary inflammation dominates independently of mechanics. Factors like diet-induced obesity boosts mechanical load, or toxins promote oxidative stress—but they’re not primary drivers. Systemic inflammation may accelerate progression, yet mechanical elements like shear predominate in movement-induced OA.
Outlook for Your Proposed Sequence
Supine → Prone → Back to Supine (heel-press exploration → prone leg lift → return to supine heel-press with new awareness)
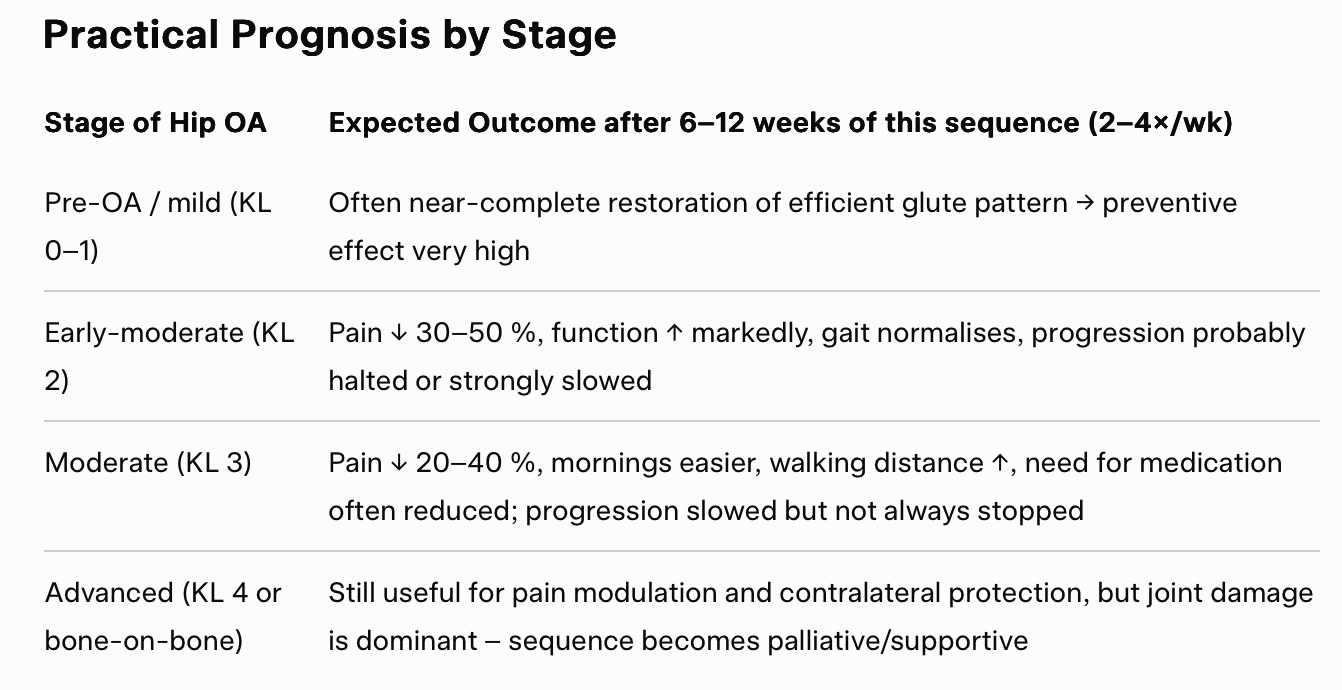
For clients with early-to-moderate hip osteoarthritis (Kellgren-Lawrence 1–3, no acute flare), this is one of the smartest, most evidence-aligned somatic sequences you can run. It directly targets the exact mechanical fault we just discussed (insufficient posterior glide / anterior shear from poor glute recruitment) while staying 100 % within Feldenkrais principles (non-forcing, constraint-led discovery, awareness-based).

